NHS Heath Check e-Bulletin - World Heart Day
Today is World Heart Day– a great opportunity for the Cardiovascular disease (CVD) community to unite in the fight against CVD. Cardiovascular disease is the number one leading cause of death globally, and in England CVD causes 1 in 4 deaths which equates to 1 death every 4 minutes. It also disproportionately affects our poorest communities, with people living in the poorest parts of England four times more likely to die prematurely than those in the most affluent areas.
This special e-Bulletin focuses on the national CVD ambitions and includes articles from charities on atrial fibrillation, blood pressure and cholesterol as well as updates on national projects such as CVDPREVENT and the Accelerating Disease Detection (ADD) project. We’ve also collaborated with Health Awareness 2020 to contribute to their CVD feature in The Guardian.
Please do join the discussion on twitter #worldheartday #nhshealthcheck #cardiovascularHealth #zeroCVD
Keeping the beat: getting to the heart of detection and management
Katherine Thompson, Head of the Cardiovascular Disease Prevention Programme, Public Health England
@thomp_katherine

Over the last 40 years, there have been dramatic reductions in deaths from cardiovascular disease (CVD). A tremendous achievement in its own right, these reductions have also made a significant contribution to increases in life expectancy.
While this means that many of us will benefit from living longer, those extra years of life are likely to be spent in poor health. Unfortunately, CVD also has a role to play here, affecting the lives of nearly seven million people.
CVD doesn’t affect everyone equally. People living in England’s most deprived areas are disproportionately affected. It is also more common among men, older people, people with a severe mental illness and among South Asian or African Caribbean communities. This not only bears a great cost to those affected, but health care costs are estimated at £7.4 billion and those to wider society at £15.8 billion per annum.
National CVD ambitions
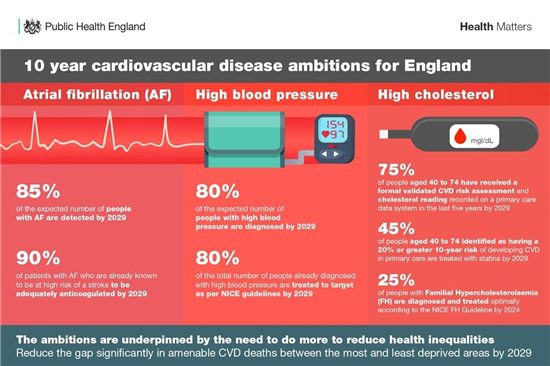
Given that most CVD conditions are preventable, there is a considerable opportunity to make a difference. Bringing together over 40 health and social care partners, Public Health England has facilitated the development of national CVD ambitions. These focus on improving the detection and management of three common CVD conditions: atrial fibrillation, high blood pressure and high cholesterol. Optimal management of these conditions can be very effective at preventing heart attacks and strokes. However, late diagnosis, under treatment and unwarranted variation in care is common.
Benefits of improving secondary prevention
Many organisations have already recognised the value of taking action on atrial fibrillation, hypertension and high cholesterol, as highlighted in our 10 year CVD national ambitions - one year on blog. However, we are not there yet and these concerted efforts need to continue. New data on the NHS Health Check programme shows that between 2012 and 2017 for every four checks delivered one person was identified as being at risk of CVD, and one was diagnosed with hypertension. For every three checks one person had an abnormal cholesterol result. Similarly, an updated evidence review highlights that the programme does result in the increased detection of disease as well as increases in statin prescribing and reduction in some risk factors six years after a check. The evidence indicates that NHS Health Checks can play a crucial role in both reducing risk and detecting disease. However, it’s impact can only be maximised if it is delivered in a way that encourages more people to have a check and ensures that they then get the opportunity to benefit from appropriate behavioural and clinical intervention.

PHE estimates show that if we can bring the national ambitions about, within three years, then at least 49,000 strokes and 32,000 heart attacks could be prevented, making a substantial contribution to NHS England’s commitment to save 150,000 heart attacks, strokes and cases of dementia over 10 years. Over 10 years, the societal return on investment is estimated to be £2.30 for every £1 spent, including the value placed on improved health.

Further action
England has the potential to become a world leader, but doing so requires action by the NHS, local authorities, and charities to utilise a range of delivery approaches, including:
- strengthening the NHS Health Check to support early diagnosis and management;
- Integrated Care Systems developing and delivering new CVD prevention models of care;
- implementing NHS England’s RightCare CVD prevention pathway;
- using existing data to make the case for action;
- making positive behavioural changes for preventing CVD;
- raising public awareness of CVD risk factors and opportunistic detection.
Saving your life can be as easy as one, two, three
Trudie Lobban MBE, FRCP Edin, Founder of Arrhythmia Alliance & AF Association

Atrial fibrillation (AF) is the most common form of arrhythmia (irregular heart rhythm), affecting one in four aged 65 or older. It occurs when the chambers of the heart do not beat in rhythm, causing a rapid and irregular heart rhythm. The symptoms of AF can include palpitations, shortness of breath, exhaustion or feeling dizzy.
While these symptoms may be unpleasant, the real danger with AF is the risk of AF-related stroke. AF patients have a five-fold increased risk of AF-related stroke and are more likely to have a more severe stroke — 60% of those who do have an AF-related stroke will become disabled and 20% will die.
Therefore, assessing the risk of an AF-related stroke is vitally important so that, if necessary, they can take anticoagulation therapy to reduce their risk of an AF-related stroke. However, another issue is that some AF patients do not have any symptoms or have such mild symptoms that they do not seek medical attention. This means that they can be going about their daily life completely unaware that they are in danger of having an AF-related stroke. In fact, some people are only diagnosed after experiencing an AF-related stroke.
For this reason, the AF Association, along with its sister charity, Arrhythmia Alliance, runs the “Know Your Pulse” campaign. The aim of this campaign is to encourage people to know their pulse to know their rhythm, so that they can act if they find that their pulse rhythm is irregular. We believe thousands of lives could be saved — through the prevention of AF-related stroke — if pulse checks became routine. Therefore, highlighting the importance of pulse rhythm being checked as a routine part of a blood pressure reading during an NHS Health Check
We have a host of resources, including videos, showing people how easy it is your take your pulse to know your heart rhythm. We say that taking your pulse is as “easy as one, two, three” and could quite literally save your life. To find more about the work of the AF Association, visit: www.heartrhythmalliance.org/afa/uk/
Know Your Numbers to Beat CVD
Katharine Jenner, CEO of Blood Pressure UK

At Blood Pressure UK, the UK’s leading blood pressure charity, we have always known the importance of Knowing Your Numbers to help beat cardiovascular disease (CVD), which is why for the last 20 years, we have encouraged health professionals to undertake blood pressure testing, in the community, in pharmacies and through NHS Health Checks. We want to find the missing millions of people in the UK that have high blood pressure but don’t even know it, and advise them on how to lower it, and their risk of CVD.
In the UK, high blood pressure already costs the NHS over £2.1 billion every year through the heart disease, heart attacks and strokes it causes, yet 6.5 million people remain undiagnosed. According to Office for National Statistics data, in the last two months alone the number of deaths caused by high blood pressure in those aged under 65 is up by one third. It is therefore vital that we identify those living with high blood pressure and help them bring it under control.
Home monitoring is one way of doing this and is strongly recommended by the UK’s National Institute for Health and Care Excellence. This is why we have asked the UK Secretary of State for Health for home blood pressure monitors to be made available on prescription to anyone who has been diagnosed with high blood pressure.
2020 marks the 20-year anniversary of the charity and has coincided with a time when taking control of our hearts and our health has arguably never been more important. Until access to GPs and other healthcare professionals, and NHS Health Checks are less restricted due to the coronavirus pandemic, home blood pressure monitoring is a great opportunity to take control of our health.
We are delighted to have been able to create new, free and simple to use guides, videos and information for anyone that wants to try home blood pressure monitoring – please encourage your family and your friends to do the same, so we can beat CVD.
HEART UK – Let’s talk about cholesterol
Simon Williams, Head of Communications & Policy, HEART UK - The Cholesterol Charity

Over half of all adults in England have raised cholesterol (>5mmol/L). We need cholesterol in our blood to stay healthy, but too much can lead to serious health problems in the future, including heart attacks and strokes.
HEART UK is the UK’s only Cholesterol Charity. We provide expert support, education and influencing services to healthcare professionals and people and families with concerns about cholesterol. Our free HEART UK professional membership area contains up to date research, journals and news as well as providing the opportunity to network with other health professionals interested in blood fats and CVD. In addition, we have recently started a series of monthly podcasts on a range of topics from the impact of COVID-19 and cholesterol, to fashionable diets such as the keto diet and have partnered with Diabetes UK and Blood Pressure UK.
Our website has a wealth of patient information that offers scientifically backed information in a practical and every-day way that Healthcare professionals can signpost patients to. For example, patients are often apprehensive about certain medication, especially given the abundance of falsehoods made. We provide further supporting information on the range of cholesterol lowering treatments that are factually accurate and scientifically based for patients to make more informed choices about taking lifesaving medication.
All the information and support we offer is available without charge for the public. With our cardiac nurses, specialist cardiac dietitians and access to specialist lipidologists available on a telephone helpline, and increasingly more by email, we hope to offer the support to those that need it to better manage their cholesterol, often following an NHS Health Check.
October is our National Cholesterol Month and the campaign this year is to encourage people to talk about cholesterol. For most people knowing what their cholesterol levels are is the first step in avoiding a heart attack or stroke and we hope to reach a million people in this campaign, encouraging them to also get a NHS Health Check.
Find out how much you know about cholesterol and try out our Clued-up About Cholesterol Quiz.
National cardiovascular disease audit to start in primary care
Lorraine Oldridge, National Cardiovascular Intelligence Network (NCVIN), Public Health England

A nation-wide audit will help primary care to understand how many patients they have with high-risk conditions such as high blood pressure, atrial fibrillation and high cholesterol or existing cardiovascular disease, who are potentially undiagnosed, under- or over-treated.
Preventing 150,000 strokes and heart attacks
The audit (CVDPREVENT) will see NHS England & Improvement, NHS Digital and Public Health England (PHE) working together to provide new national cardiovascular data to underpin quality improvement initiatives in primary care.
It will support both the NHS Long Term Plan ambition to prevent 150,000 strokes and heart attacks over the next ten years, and the CVD prevention element of the upcoming Directly Enhanced Service specification in 2021/22.
Highlight gaps, identify inequalities
CVDPREVENT will provide a foundation for professionally-led quality improvement, in individual GP practices across Primary Care Networks (PCNs). It will provide data to highlight gaps, identify inequalities and monitor improvement and impact on inequalities, as well as enabling and guiding opportunities for improvement.
The audit will extract information, that is already routinely collected in primary care, without any additional burden to GP practices. Data will be extracted for individuals who either have existing cardiovascular disease or who have one or more of the following six high-risk conditions: atrial fibrillation, high blood pressure, diabetes, non-diabetic hyperglycaemia, chronic kidney disease, familial hypercholesterolaemia and other hyperlipidaemias. It will also extract data for individuals with an entry in their record that may suggest that they have an undiagnosed high-risk condition.
Addressing health inequalities
While individuals will not be identifiable from the data, the collection of record-level data on demographics, ethnicity and gender will allow the assessment of the impact of quality improvement on health inequalities. This is particularly important as CVD contributes to the disparity in health outcomes between rich and poor, accounting for 25% of the total gap in life expectancy.
More information is available at: https://www.england.nhs.uk/ourwork/clinical-policy/cvd/cvdprevent/
The UK’s largest ever health research programme begins recruitment in early 2021
Accelerating Detection of Disease - the UK’s largest ever health research programme - is set to begin recruitment in pilot areas in early 2021.
Today, millions of people in the UK and around the world spend many years of their later life in poor health. By developing a more detailed understanding of what makes certain people more likely to develop a disease, plus what to look out for before any symptoms appear, the Accelerating Detection of Disease (ADD) programme offers the potential to help to develop far more effective approaches to both prevention and treatment.
ADD is designed to help researchers find out as much as possible about how health changes as people age, by tracking back to find the earliest signs of common diseases such as dementia, cancer, diabetes, heart disease and stroke. The aim is to build a cohort of 5 million volunteers over the age of 30 by 2024 that truly reflects the UK population. Building this large and diverse cohort will provide researchers from universities, charities, the NHS and companies involved in health research with new opportunities to identify differences in how diseases such as dementia, cancer, diabetes, heart disease and stroke begin and progress in people from all types of backgrounds.
For the pilot phase, the ADD team are keen to work with GP practices in around five local authorities. Following the pilots, the aim is to expand participation right across the UK for the main phase of the programme, beginning later next year.
Join us for a webinar on Monday 5th October, 13:00 – 14:00 to hear more about the programme and the opportunity to be one of the pilot areas helping establish this world-leading resource for health research. The webinar will be led by Professor John Deanfield and Claire Levermore, Director of Operations for the programme.
CVD Prevention Webinar Series
Our Cardiovascular Disease webinar series has now restarted, you can subscribe to our webinar mailing list here. Upcoming webinars include:
- NHS Health Check digital exemplar: learning from the discovery phase - 09 October 2020, 11:00–12:00
- Influences on NHS Health Check behaviours: a systematic review - 22 October 2020, 09:30–10:30
- NHS Health Check evidence review 2020 – 05 November 2020, 14:00 – 15:00
- NHS Health Check Data extraction analysis – 18 November 2020, 13:00–14:00
You can find the presentations and videos for past webinars here.
Please note webinar times are subject to change.